The protective role of vitamin D in BNT162b2 vaccine-related acute myocarditis
-
An interesting study from China.
The protective role of vitamin D in BNT162b2 vaccine-related acute myocarditis (2025)
Results: A high incidence of hypovitaminosis D (73.3%) was observed in these individuals with vaccine-related myocarditis, particularly in those presented with chest pain or intensive care unit (ICU) admission. Moreover, vitamin D level was negatively associated with peak serum cardiac troponin T level during vaccine-related myocarditis. Genotypically, the GC (vitamin D binding protein) rs4588T allele which encoded the GC2 isoform of vitamin D binding protein was a risk allele, whereas the GC1S isoform was protective. Mechanistically, hypovitaminosis D was associated with higher levels of cytokines pivotal for natural killer (NK) cells (particularly interleukin-1β (IL-1β), IL-12, Interferon-γ (IFN-γ), and IL-8) and higher percentage of CD69+ NK cells in blood, which in turn correlated with chest pain presentation.
Conclusion: These data support the hypothesis that vitamin D plays a crucial role in mitigating mRNA vaccine-related myocarditis by modulating proinflammatory cytokine milieu and subsequent unfavorable NK cell activation, laying a groundwork for preventive and treatment strategies.
-
And from Thailand:
Association Between Vitamin D Levels and Long COVID Signs and Symptoms (2025)Results: The study results indicated a female-to-male ratio of 1.1:1 and a mean age of 45.87 ± 8.65 years; of these, 62.4% received three doses of the COVID-19 vaccine, and 64.7% developed long COVID. The most prevalent signs and symptoms were respiratory (55.3%), skin (50.6%), and general (39.4%). The median blood vitamin D level was 22.96 ng/mL, with 41.2% of subjects having insufficient levels, 30.6% having deficient levels, and 28.2% having sufficient levels. Patients with long COVID had significantly lower vitamin D levels compared with those without long COVID (21.52 ng/mL vs. 25.46 ng/mL; p < 0.05). Multivariable analysis found that vitamin D deficiency was significantly associated with overall long COVID signs and symptoms (Adj. OR, 5.80 [95% CI: 2.10, 16.13]). Additionally, vitamin D deficiency significantly increased the number of long COVID systemic signs and symptoms (Adj. IRR, 3.30 [2.12, 5.12]).
Conclusion: Assessing and maintaining vitamin D levels, vitamin D supplementation, and sunlight exposure in COVID-19 patients can reduce the risk and severity of long-term COVID-19 signs and symptoms.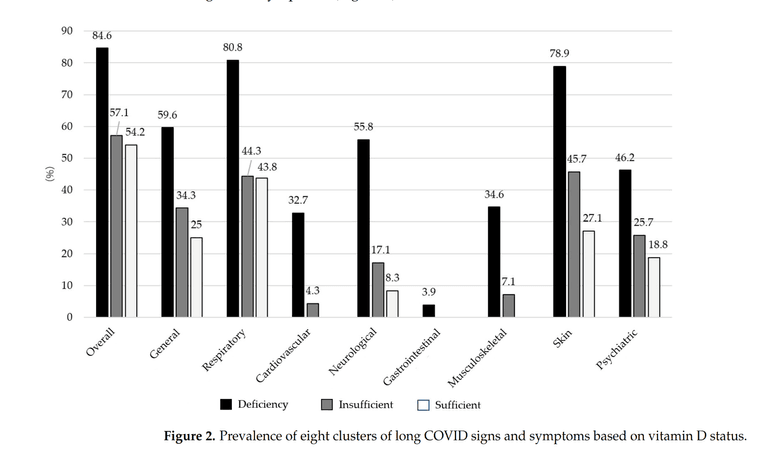
Hello! It looks like you're interested in this conversation, but you don't have an account yet.
Getting fed up of having to scroll through the same posts each visit? When you register for an account, you'll always come back to exactly where you were before, and choose to be notified of new replies (either via email, or push notification). You'll also be able to save bookmarks and upvote posts to show your appreciation to other community members.
With your input, this post could be even better 💗
Register Login