The entire cardiovascular system, not just the heart, form vortexes. Optimize these vortices via exercising in gravity.
-
Fluid dynamics of vortex patterns involves the study of rotational flow structures where fluid particles move in helical or circular paths around an axis, creating coherent, energetic structures. These localized regions of rotational motion, characterized by high vorticity—the curl of the velocity field—are essential to understanding turbulence, shear flow, and transport processes in both engineering applications and natural phenomena.
Vortex Formation in the Cardiovascular System
https://www.researchgate.net/publication/229068637_Vortex_Formation_in_the_Cardiovascular_System
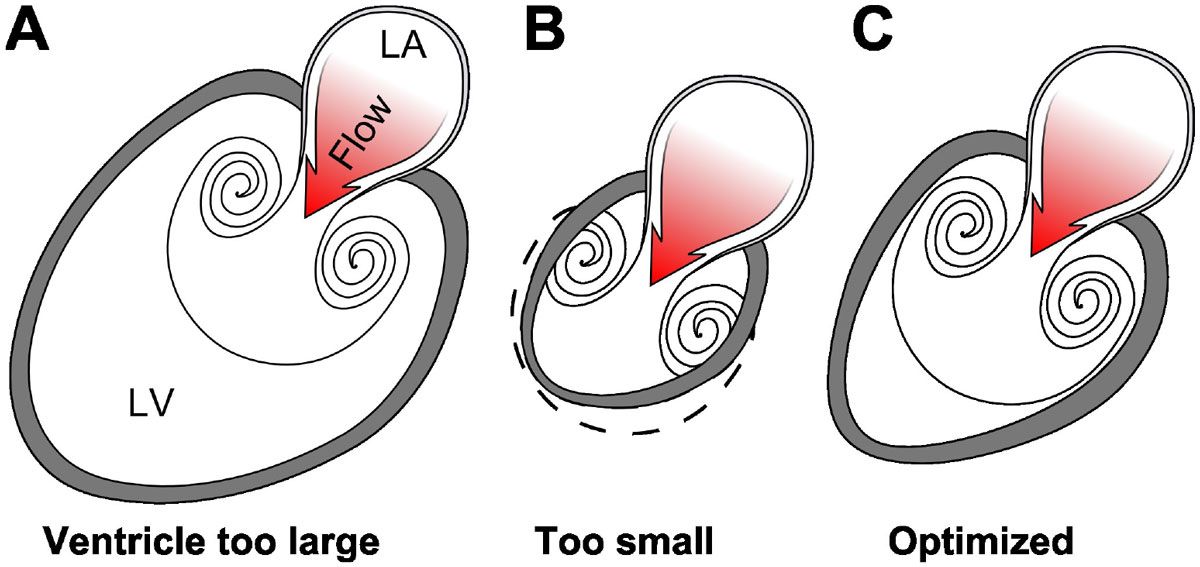
Full PDF: https://users.encs.concordia.ca/~kadem/MECH691X/VortexFormationInTheCardiovasc.pdfThe shape of the healthy heart is optimized for vortex ring formation
https://pmc.ncbi.nlm.nih.gov/articles/PMC5032082/Cardiovascular Research by Leonardo da Vinci (1452–1519)
https://www.ahajournals.org/doi/10.1161/CIRCRESAHA.118.314253Viktor Schauberger (1885–1958) was an Austrian naturalist who developed "implosion technology," focusing on natural, spiraling water vortices to generate energy, purify water, and create lift.
https://en.wikipedia.org/wiki/Viktor_SchaubergerStudy Finds Astronauts’ Hearts Become More Spherical in Space
"heart becomes more spherical when exposed to long periods of microgravity in space, a change that could lead to cardiac problems"
The astronauts’ more spherical heart shape appears to be temporary, with the heart returning to its normal elongated shape shortly after the return to Earth. The more spherical shape experienced in space may mean the heart is performing less efficiently, although the long-term health effects of the shape change are not known.
https://www.acc.org/about-acc/press-releases/2014/03/29/09/09/may-hearts-in-spaceWall shear stress and its role in atherosclerosis
The onset of plaque usually occurs in the low WSS area, and the plaque development alters the local WSS topography. low WSS promotes atherosclerosis, while high WSS prevents atherosclerosis. Upon further progression of plaques, high WSS is associated with the formation of vulnerable plaque phenotype.
https://www.frontiersin.org/journals/cardiovascular-medicine/articles/10.3389/fcvm.2023.1083547/fullCardiovascular Effects of Exercise: Role of Endothelial Shear Stress
The notion that regular aerobic exercise reduces cardiovascular morbidity and mortality in the general population as well as in patients with coronary artery disease is strongly supported by evidence derived from epidemiologic studies (1., 2., 3.). Physically active people also experience fewer clinical manifestations of coronary artery disease than do less active men and women (4). By contrast, sedentary life-style has been identified as a risk factor for development of coronary artery disease, and there is a strong correlation between physical inactivity and cardiovascular mortality (3,5). Although vigorous physical exertion is a precipitating factor for myocardial infarction, this adverse outcome is usually incurred by persons who otherwise lead a sedentary existence (6,7). Consequently, daily physical aerobic activity is considered an effective component of both primary and secondary prevention of cardiovascular events (8,9).
https://www.sciencedirect.com/science/article/pii/S0735109796003932Sitting and endothelial dysfunction: The role of shear stress
Sedentary activity results in low SS in the lower extremities which may result in increased oxidative stress and impaired endothelial function. This review furthers the use of sitting as model to study the effects of inactivity, discusses possible physiological mechanisms and suggests future directions.
https://pmc.ncbi.nlm.nih.gov/articles/PMC3560806Arterial stiffness and hypertension
Arterial stiffness and hypertension are closely related in pathophysiology. Chronic high blood pressure (BP) can lead to arterial wall damage by mechanical stress, endothelial dysfunction, increased inflammation, oxidative stress, and renin–angiotensin–aldosterone system (RAAS) activation. Hypertension also increases collagen fiber production and accelerates elastin fiber degradation. Stiffened arteries struggle with BP changes, raising systolic BP and pulse pressure. The resulting increased systolic pressure further hardens arteries, creating a harmful cycle of inflammation and calcification. Arterial stiffness data can predict target organ damage and future cardiovascular events in hypertensive patients. Thus, early detection of arterial stiffness aids in initiating preventive measures and treatment plans to protect against progression of vascular damage. While various methods exist for measuring arterial stiffness, pulse wave velocity is a non-invasive, simple measurement method that maximizes effectiveness. Healthy lifestyle changes, RAAS blockers, and statins are known to reduce arterial stiffness. Further research is needed to ascertain if improving arterial stiffness will enhance prognosis in hypertensive patients.
https://pmc.ncbi.nlm.nih.gov/articles/PMC10691097/Exercise and Dietary Influences on Arterial Stiffness in Cardiometabolic Disease
https://www.ahajournals.org/doi/10.1161/hypertensionaha.113.02277The Acute Effect of Exercise on Arterial Stiffness in Healthy Subjects: A Meta-Analysis
Our results show that, although there is a significant reduction in pulse wave velocity 30 min after exercise, the levels of arterial stiffness return to their basal levels after 24 h. These findings could imply that, in order to achieve improvements in pulse wave velocity, exercise should be performed on a daily basis.
https://pmc.ncbi.nlm.nih.gov/articles/PMC7831005/ -
Improving blood flow to the extremities (hands and feet) involves more than just "moving more." It requires a balance between the mechanical pumping of the heart and the biochemical signals that tell your blood vessels to open up (vasodilation).
For someone focused on metabolic efficiency, the goal is to improve circulation without triggering excessive stress responses that can actually lead to peripheral vasoconstriction.
1. The Biochemical Trigger: The Role of CO2
Effective circulation depends on the Bohr Effect. For oxygen to leave your blood and enter your tissues (especially in the small capillaries of your fingers and toes), carbon dioxide (CO2) must be present.
- Vasodilation: CO2 is a powerful natural vasodilator. When your metabolic rate is high and you are producing CO2 efficiently, your blood vessels relax, allowing blood to reach the extremities.
- The Trap: Over-exercising to the point of "gasping for air" or hyperventilating actually flushes CO2 out of the system. This can cause the peripheral vessels to constrict, leading to cold hands and feet even while your heart rate is high.
2. Strategic Exercise Selection
To optimize blood flow to the extremities, the type of movement matters.
- Resistance Training (Concentric Focus): Lifting weights or bodyweight movements (like squats or push-ups) creates a mechanical "pump" effect. Focus on the concentric (the lifting phase) to stimulate blood flow and metabolic demand without creating excessive tissue damage or systemic inflammation.
- Low-Impact Steady State (LISS): Walking at a brisk pace where you can still breathe through your nose helps maintain a high CO2 tension. This keeps the peripheral "gates" open longer than high-intensity sprinting might.
- Micro-Movements: If you spend long periods at a desk, simple calf raises or grip strengtheners are highly effective. The calves are often called the "second heart" because their contraction is essential for pumping venous blood back up from the feet.
3. Thermoregulation and the "Core-to-Extremity" Link
Your body prioritizes keeping your internal organs warm. If your core temperature drops even slightly, the body will pull blood away from your skin and extremities to protect the center.
- Warmth as a Catalyst: Exercising in a warm environment or wearing adequate layers helps signal to the nervous system that it is "safe" to send blood to the periphery.
- Metabolic Rate: A robust oxidative metabolism keeps your internal "furnace" running. If your resting metabolic rate is low, your body will naturally be more stingy with blood flow to the fingers and toes.
4. Nutritional and Biochemical Support
Circulation is also a matter of fluid dynamics and mineral balance.
- Magnesium and Calcium: Magnesium helps the smooth muscles of the blood vessels relax (vasodilation), while calcium helps them contract. Ensuring adequate magnesium intake can prevent the "clamping" of peripheral vessels.
- Sodium Balance: Adequate salt intake is necessary to maintain blood volume. Low blood volume makes it much harder for the heart to push blood all the way to the ends of the limbs.
- Short-Chain Fatty Acids (SCFAs): Compounds like butyrate can support mitochondrial health and gut integrity, which indirectly supports systemic blood flow by reducing the low-grade inflammation that can make vessels "stiff."
Summary of Strategies
Strategy Action Mechanism Nasal Breathing Breathe only through the nose during light exercise. Increases CO2 retention and vasodilation. Calf Raises Perform 20 reps every hour while sitting. Engages the "venous pump" in the lower legs. Temperature Check Keep the torso and neck warm. Prevents the "survival" vasoconstriction reflex. Mineral Balance Ensure sufficient Magnesium and Salt. Maintains blood volume and vessel flexibility.