Bile can serve as a reservoir for funghi, making them harder to treat
-
@CrumblingCookie nystatin is pretty weak ime but i guess it depends on which fungi
ketoconazole cream works way better ime but idk what strains it is working agaisnt. i think mallesseziaberberine seems interesting, is it peaty ? it isnt right, because it is like metformin and metformin isnt peaty
-
Thanks for sharing.
Indeed I currently find myself in a situation wherein I don't know for how long in total to continue fluconazole. Months? It costs about $60/week for me. And it's difficult to say which depressive mental effects are true sides and which are due to various degrees of die-off.
I wonder what role the continous re-infection from bile plays in commonly required treatment length. The notion of it being impossible to clear from tissues is what I find unsettling, too.
Have started to add in berberine today, 500mg thrice daily. Along with ample propolis extract twice daily.
Luckily I've failed to make it to the store in time and stumbled upon some garlic in my kitchen drawers and have read up on allicin again.
One half to a full garlic bulb per day is allegedly a good guideline for powerful effects (about 1mg allicin per kg BW from 3-5mg allicin per g fresh garlic). Ground it/crush it, let it rest for 10 minutes for the allicidase to do its work before diluting it in food or adding any acids like vinegar.@sunsunsun said in Bile can serve as a reservoir for funghi, making them harder to treat:
iron chelation in fungi via doxycycline makes fluconazole anti fungal against some candida rather than just fungistatic or no effect
That study is in-vitro and super misleading however, because few antibitiocs, if any other at all, are as fungal-infection promoting as the tetracyclines because of their powerful, continuous inhibition of phagocytosis lasting for days even after stopping further intake. Tetracyclines are one of the main risk factors for fungal infections in literature. Ime they are very overhyped and terrible.
As for ketoconazole I'm wary of its unique VDR antagonism which essentially inhibits innate immunity and reduces xenoautophagy of intracellular endomyceles. That also essentially makes ketoconazole topical creams a powerful antiinflammatory for skin conditions, saving the extra prednisolone so enamored by dermatologists.
-
-
@sunsunsun Wax moths? They don't even have neutrophils and I won't deep-dive into finding out how their hemolymphs specifically compare to human or mammalian neutrophils.
I really do harbor strong apprehensions against the potential (mis)use of doxy on fungal infections.What I would much rather do is oral terbinafin + fluconazole.
The terbinafin by itself is useless against many fungi species but by disturbing an earlier point (Erg1) in the sterol biosynthesis pathway it is synergistic with azoles (which act upon Erg11).
allegedly it strongly inhibits expression of the fungal efflux pumps responsible for azole resistance!
(! Berberine is the one which inhibits efflux pump expression. I had mixed it up).
This still won't tackle activitiy in the biliary tract, though.I've done some more reading of publications on biliary / gallbladder candida / fungi.
Fungi can be causes of calculous (lithiasic) or also acalculous cholecystitis with or without mixed bacterial infections (Escherichia coli, Enterococcus, Klebsiella, Enterobacter, Clostridia).
Even in such rare and often fatal cases that happened to be documented, candidemia was rare despite frequent (almost always) fungal infection of other organs.https://pubmed.ncbi.nlm.nih.gov/8862389/
https://pubmed.ncbi.nlm.nih.gov/28703118/
https://pmc.ncbi.nlm.nih.gov/articles/PMC8764969/
https://pmc.ncbi.nlm.nih.gov/articles/PMC12338181/
https://pubmed.ncbi.nlm.nih.gov/24474028/
https://pubmed.ncbi.nlm.nih.gov/8207288/I don't have visible gallbladder wall thickening or distention or an obviously, universally accepted liver disease (except for hepatomegaly) but if I had I sure as hell would want to insist on flucytosine, or flucytosine + i.v amphotericin B along with any broad-spectrum antibiotics and before mutilating surgeries they'd offer.
Have looked more into berberine again, too. It's impossible to achieve its antimicrobial concentrations (at least 0.1mg/mL) systemically. Serum concentrations are about 0.5 - 16 ng/mL. I.e. 0.000005 mg/mL. Ridiculous!
The berberine in practical doses of 500-1500mg will thus be acting mainly within the GI lumen in support of oral Ampho-B. Berberine has low absorption but some will spill over to reach the liver for extensive first-pass metabolism, yet probably not into biliary ducts. -
Great points, guys.
My current working hypothesis is rotating and combining several anti fungals daily + keeping bile flowing.
If i don't rotate the antifungals they seem to loose effect surprisingly quickly.
But what is obvious from many studies, is that combining certain anti fungals can drastically increase their effectiveness. Nystatin is synergistic with thymoquinone and also thymol IIRC.The other important part is to keep bile flowing and excreting it. The lowtoxin crowd actually has a point there. Inducing a bile dump seems very therapeutic to me and followed by certain time of remission/ relieve.
So having adequate fiber intake seems important. Pectin is helpful, vitamin D and K as well.
I also ordered an herb that's used for cholestasis in TCM called Artemisia capillaris it has a lot of studies on liver health and general anti-inflammatory effects. -
@sunsunsun said in Bile can serve as a reservoir for funghi, making them harder to treat:
idk about in context of bile, but iron chelation in fungi via doxycycline makes fluconazole anti fungal against some candida rather than just fungistatic or no effect. aspirin is also an iron chelator.
Makes sense. I've been using an iron cast pan for years and my ferritin came back very high.
Maybe that contributed to my susceptibility to (fungal) infections.@sunsunsun said in Bile can serve as a reservoir for funghi, making them harder to treat:
total eradication of fungi seems impossible on a realistic sense
if bile is a reservoir for fungi maybe just eating high bile binding foods regularly can flush it out. rather than recirculating bile more
Yes agreed


-
@CrumblingCookie said in Bile can serve as a reservoir for funghi, making them harder to treat:
Any info on how methylsulfonylmethane would be antifungal?
They say it's the sulfur in it. There's not a lot of evidence for that though. From my experience it is definitely anti-fungal.
I suspect it can chelate metals. Usually that doesn't just involve the bad heavy metals but also the good ones. So Id make sure to test my minerals and keep intake high when taking it long term. -
For what it's worth, let me throw in some tidbits from what I've conjectured over my 2 decades of trying to lower my blood pressure. I've done a lot from eliminating a lot of periodontal bacteria that has translocated to my vascularure to chelating lead lately using Emeramide. Through a process of elimination of these possible causes, I have been halfway successful only though in lowering my blood pressure. From 260/160 to a current 169/110, I still have ways to go.
But I still some light at the end of the tunnel though. And it is something I have overlooked. As fungal infection has always been under the radar and an afterthought inmedical circles. Doxtors would treat bacteria with antibiotics, and rarely talk about fungus. A confinement in a hospital would see a patient get well from antiiotic administration, but a discharge would be delayed only because the good doctor for some hunch decides to give some antifungals..
I would later realize that some antibiotics are known to transform bacteria into cell wall- deficient microbes that are harder to kill because they lack this cell wall which is used to kill microbes with antibiotics. This transformation from bacterial form to a form halfway between bacteria and a fungi ia at the hear of a ' competing medical dogma called terrain theory, which is opposed to the mainstream model based on herm theory- where all microbes are accepted as being static in nature, and do not pleomorph, as would be what happens when commensal and regulatory (aka friendly bacteria) turn from Dr. Jekyll into Dr. Hyde, and become pathogenic.
But this should explain to me why it has become common practice for doctors to administer antifungal drugs after successfully treating a patient with antibiotics. But they cannot explain why, for to say the real reason is to somehow agree that terrain theory is real, which is anathema to their cornerstone germ theory.
But back to my vexing problem of fixing my high BP problem, which is on its 26th year.
Lately, I had began taking artemisia annua tincture which saw me successfully lower my BP from 200./150 to 150/100. I took this as an antifungal to hyphal aspergillosis (aspergillus niger is also known as black mold. How I got this is another story).
It would be nice if my BP kept going down to 120/80. That would be a nice end to this story.
But my BP held at around 150/100 - 160/110. I was still urinating foamy urine. And I realize that this is the result of a continuing activation of neutrophils and macrophages th as t I would conclude from my CBC test, showing my wbc to be high and my neutrophils and monocytes to be high.
Even as my eosinophils have gone down as the large hyphal aspergillus fungal parasite colony have been markedly reduced. But the fungus took on a smaller form called a clamydophore. And in this form, more neutrophils and macrophages were needed to kill or neutralize them.
This is the reason why in my CBC test, there would be a high count both in neutrophils and monoxytes.Yet Iinflammation and oxidative stresses from ROS being produced and spilling over to destroy adjacent tissues would keep occurring, and that my body would have to use its antioxidants to protect tissues from.being destroyed. The main extracellular antioxidant would be called upon again, and albumin would be oxidized and excreted in urine. Which would explain foam in my urine. As well as mynhigh BP as my albumin stores in plasma would be insufficient to hold on to salt, with salt being needed to keep my plasma and blood volume high enough. The body compensates by increasing blood pressure.
But this fungal presence is hard to destroy. As you would concur. What I am trying now, in addition to turpentine and artemisia annua, is the use of Lugol's Iodine. In the next weeks and months, I will find out.
Looking back, I can't help but see why my LDH has always been high at around 260. I think it is because I have hemolysis. Under the radar. It is from an underlying fungal presence that needs to feed off iron from red blood cells it breaks down.
Since heme oxygenase enzyme breaks down the heme from hemolyzed red blood cells, the carbon monoxide could also explain why when I look at my heart rate chart, I would see occasional transient sharp drop in my heart rate even when my spO2 chart says I have a lot of oxygen at that given time. It is because a typical.oximeter cannot distinguish carbon monoxide from.oxygen, and the carbon monoxide is masking as oxygen, even as my heart cannot use the carbon monoxide to produce energy. I have a bit of carboxyhemoglobinemia. That is how I see it. And that would be a result if an ongoing case of chronic low level hemolysis caused by iron-hungry aspergillus fungi. The same fungi that is causing high BP stealthily.
Fungi remains as a. bogeyman to us.
-
@Mauritio taurine for bile excretion actually seems better than TUDCA at their relative normal doses (3g per day for taurine vs 500mg per day for TUDCA)
-
Result or (mutualistic) cause? It's pointing to the latter!
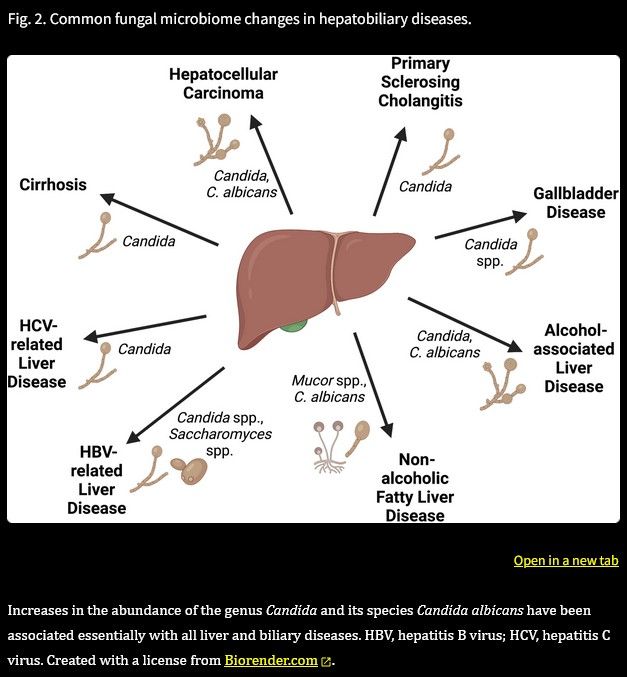
Fungal infections and the fungal microbiome in hepatobiliary disorders, 2022
@mauritio and others I urge you to read through the whole paper. It's a very scientifically sober and factual work which converges various interrelated aspects.
Excerpts (it appears almost necessary to quote the whole thing):
Although patients with cirrhosis already have elevated faecal levels of Candida [111], patients with HCC were found to have even higher faecal proportions of Candida and C. albicans than patients with cirrhosis, but lower proportions of the genera Kazachstania, Debaryomyces, Xeromyces, Amorphotheca, and Blastobotrys [122]. In a mouse model of HCC, gavage with C. albicans resulted in exacerbated HCC volume, which was dependent on the nucleotide-binding oligomerization domain-like receptor family pyrin domain-containing 6 (NLRP6) inflammasome [123]. Moreover, development of HCC in a patient with cirrhosis increases their risk of oesophageal candidiasis (OR 10.04) [113].
Specific serum anti-C. albicans IgG and IgM titres are increased in patients with AUD vs. controls, and interestingly, the anti-C. albicans IgG titre (but not the IgM titre) decreases significantly in patients after abstinence [55]. These changes parallel elevated faecal proportions of C. albicans in patients with AUD (vs. controls), which decrease after abstinence [55]. Similarly, plasma anti-C. albicans IgG titres are increased in patients with NAFLD and advanced fibrosis (F3-F4) vs. patients with NAFLD and no/early fibrosis (F0-F2) and vs. controls, and anti-C. albicans IgG titres correlate with the faecal C. albicans/S. cerevisiae log ratio [56]. Anti-C. albicans IgG titres hence correlate with disease activity in ALD [55] and NAFLD [56], indicating more systemic exposure to C. albicans in more severe liver disease.
Candidalysin is a secreted cytolytic peptide toxin from C. albicans that directly damages epithelial membranes, triggers a danger response signalling pathway and activates epithelial immunity [129]. C. albicans strains lacking this toxin do not activate or damage epithelial cells and are avirulent in animal models of mucosal infection [129]. The extent of cell elongation 1 (ECE1) gene encoding candidalysin was more frequently present in the stool of patients with AH than AUD [98]. Further, mice gavaged with wild-type ECE1-positive C. albicans had significantly higher serum alanine aminotransferase (ALT) levels, hepatic triglycerides and inflammation than mice gavaged with ECE1-negative C. albicans in a 2-week ethanol binge model, supporting the notion that ECE1-positive C. albicans exacerbates ethanol-induced steatohepatitis in mice [98].
Secretory IgA also binds ECE1-derived candidalysin, though this binding is reduced in patients with Crohn’s, indicating fungi-related immune dysregulation [130].
Antifungal treatment improves liver disease in various mouse models, including ethanol- and western diet-induced steatohepatitis [56, 97, 131]. Further, colonisation with C. albicans [98, 123] or Malassezia restricta [99] exacerbates liver disease. Therefore, fungi and their products contribute to liver disease.
Chronic alcohol administration increases mycobial populations and the translocation of fungal beta-glucan into the systemic circulation in mice [97, 131]. Oral administration of the antifungal amphotericin B reduces faecal fungal overgrowth and beta-glucan translocation [97]. Antifungal treatment with oral amphotericin B or caspofungin prevents ethanol-induced liver disease in mice without changing plasma bacterial lipopolysaccharide levels [97, 131].
Beta-glucan induces liver inflammation via CLEC7a on Kupffer cells, as shown in experiments employing bone marrow chimeric mice [97]. CLEC7a-dependent activation of caspase-1 via NLRP3 [134, 135] leads to increased inflammatory IL-1β expression and secretion, which subsequently contributes to hepatocyte damage and ethanol-induced liver disease [97]. CLEC7a also plays a role in diet-induced steatohepatitis, since its hepatic expression is significantly increased in patients with NASH and mice on a high-fat diet, whereas Clec7a-deficient mice and mice treated with a Clec7a-antagonist are protected from diet-induced steatohepatitis and fibrosis [136].
Rats infected with C. albicans by intraperitoneal injection develop hepatic steatosis, increased serum ALT levels, inflammatory markers, and pronounced lipid peroxidation [137]. This raises the question of how C. albicans causes liver disease. One effector could be its secreted cytolytic toxin candidalysin. Candidalysin exacerbates ethanol-induced liver disease and is associated with increased mortality in mice [98]. Candidalysin does this independently of Clec7a
Candidalysin can damage primary hepatocytes in a dose-dependent manner in vitro and is associated with liver disease severity and mortality in patients with AH [98]
The PGE2-producing fungus Meyerozyma guilliermondii was increased in mice with ethanol-induced steatohepatitis [131]. Further, supplementation with Meyerozyma guilliermondii worsens ethanol-induced liver disease
Concurrent administration of an antifungal also abrogates PGE2 formation and ethanol-induced liver disease [131].
Moreover, C. albicans is a potent inducer of the Th17 response via PGE2; PGE2 is induced by the C. albicans components mannan and β-glucan that are recognised by the mannose receptor and the Clec7a/Tlr2 pathway, respectively [147, 148].
C. albicans has evolved the capacity to produce PGE2 from arachidonic acid to promote its own colonisation in the host gut [152–154]. C. albicans mutants lacking PGE2 production (genetically missing ole2, a fatty acid desaturase) are unable to colonise the murine gastrointestinal tract
Key points:
Despite a relatively small number of fungal cells in the human body, fungi are involved in the development of liver and biliary diseases.
Various rodent models of fungal microbiome (mycobiome) modulation, including increasing the fungal burden (e.g. colonisation with fungi) or decreasing the fungal burden (i.e. via antifungals), have demonstrated the impact of the mycobiome on hepatobiliary conditions.
Fungal products including toxins and metabolites can exacerbate liver and biliary diseases.
In particular, the genus Candida and the species Candida albicans play a central role in the pathogenesis and progression of essentially all hepatobiliary conditions.
Serum antibodies against fungal populations have predictive value with regard to disease severity and survival in hepatobiliary diseases.
Conclusions
Mycobiome changes have now been established in essentially all hepatobiliary conditions. However, they are still a kind of dark matter, as we often do not know their true identity and characteristics, since we cannot culture many of them.
Further, they do not colonise mice easily, so we do not have good mouse models. Nevertheless, we know that some fungi are hepatotoxic themselves and not just bystanders – for example, rodents colonised with C. albicans develop liver disease without additional stimuli.
Fungi might hence possibly exacerbate liver disease in a two-hit model, one hit being alcohol, western diet, or a toxin, and another hit being the presence and deleterious impact of fungi.
We are learning more and more about the mechanisms by which fungi contribute to liver disease, be it via fungal cell wall components or secreted toxins, such as beta-glucans or candidalysin, or fungal metabolites including prostaglandins.Wild! Profound implications for clinical practice and the foundational models of hepatobiliary diseases!
-
@CrumblingCookie there is a study showing pancreatic cancer patients usually have a fungal infection of the pancreas
and secondly, there is a case report of elevated liver enzyme ALP going down after anti fungal treatment in suspected fungal infection. this is with the generally liver toxic anti fungal drug.
-
@sunsunsun Yes, yes! The clinical neglect and snotty obfuscation into esoteric quackery is maddening!
Will update soon on what I'm doing. -
@CrumblingCookie thanks for sharing!
Very interesting. Let us know how your anti fungal cycle goes. I might try some stronger anti fungals ,too. -
@sunsunsun said in Bile can serve as a reservoir for funghi, making them harder to treat:
there is a study showing pancreatic cancer patients usually have a fungal infection of the pancreas
I found this study.
The microenvironment of a pancreatic tumor has a distinct micro biome including bacteria and fungi. Fungi are increased in mice and human samples with pancreatic cancer. Malassezia was the most prevalent species (interestingly most people with hair loss have a scalp infection of it)They found that fungi caused cancer growth!
"...the fungal mycobiome promotes pancreatic oncogenesis (11)."And more importantly, killing that fungus stopped cancer growth!
"Ablation of mycobiome with antifungal medications, such as amphotericin B or fluconazole, protected mice against oncogenic progression."Has this been tried in humans ?
This should be another reason why Haiduts anti cancer protocol works, high dose B3 and Aspirin are anti fungal.P.S. the authors also mention how bacteria influence tumor progression.
https://pmc.ncbi.nlm.nih.gov/articles/PMC7607088/"PDA tumors harbored a ~3000-fold increase in fungi compared to normal pancreas in both mice and humans."
https://pmc.ncbi.nlm.nih.gov/articles/PMC6858566/Itraconazole inhibits proliferation of pancreatic cancer cells through activation of Bak-1
https://pubmed.ncbi.nlm.nih.gov/30260036/Pancreatic cancer patient was already admitted to palliative hospital. Then received itraconazole, the tumor became operable, survived several years.
"After he received his nine-month course of itraconazole, the pancreatic cancer was readdressed and he was then deemed to be resectable and had a Whipple procedure. Over the next several years, he showed no evidence of pancreatic metastases or relapse."
https://pubmed.ncbi.nlm.nih.gov/25670260/ -
@Mauritio high dose niacinamide is not nearly as effective in vivo for dogs against what im pretty sure is mallessezia compared to a normal dose of fluconazole. and ketoconazole seems about the same as fluconazole. no experience with itraconazole but will prob try it at some point, it is very expensive in north america or europe. just observations not really scientific. in humans iirc terbinfine might be pretty good for mallessezia but in dogs they excrete it too quickly apparently.
if a dog has itchy ear , one dose of fluconazole will knock it out for a couple weeks. no need to give everyday.
imo cancer patients could probably all try an antimicrobial protocol with an antibiotic, antifungal, and antiparasite drug. reaearchers keep looking for a side target of the above drugs but im guessing the actual antimicrobial part is probably anticarcinigenic
i also have seen evidence anti serotonin drugs are anti parasite. theres a study on cyproheptadine being an anti parasite drug, from https://www.cabidigitallibrary.org/doi/full/10.5555/19900860028?__cf_chl_tk=ThtQHEaB7fbCcC9qnD19tIV6PYSAm9plCdzDERWJ0R0-1775529914-1.0.1.1-pMIrmBv2QC7gUB4mLmBDUGspQSWjaQ7agFuosFIZ.fI
-
The late and great Travis believed that boron is antifungal and that's why borax often works against arthritis. I wonder if reasonable qualities of borax could help kill fungi in the body. Travis believed so
-
@Ecstatic_Hamster Late Travis? Is he dead?
-
@Ecstatic_Hamster said in Bile can serve as a reservoir for funghi, making them harder to treat:
The late and great Travis believed that boron is antifungal and that's why borax often works against arthritis. I wonder if reasonable qualities of borax could help kill fungi in the body. Travis believed so
Good idea. My knees are sore and there are many reasons to make if sore. But it is as context specific just as it is for high blood pressure.
I need to add borax to my daily supplements to see if this works.
-
How much borax is a daily dose you woukd recommend?
-
@Mauritio said in Boron supplements:
What symptoms did you see improvement with ?
I had been taking:
Amphotericin B (per os), 100mg, four times daily
Nystatin 1 mn IU, three times daily
Borax 5g/L in drinking water for 7 days,
Itraconazole 200mg pd for 8 days, followed by
Fluconazole 200mg pd (400mg initially) for 12 days
Berberine 500mg, three times daily
Propolis extract, c. 1200mg, twice daily
1 bulb of squeezed fresh garlic pd
Simeticone 250mg once to twice daily to ease the garlic-induced flatulence,
Trans-resveratrol 500mg, twice daily
Bidifobacteria & lactobacilli blend, 1 bn, twice daily
Clostridium butyricum myairi, 600 mn three times dailyEffects of the added AmB, Nys, Itr / Flu were:
+ Halving of daily BMs (and no more liquid diarrhea), - but all associated issues remaining
+ Significant decrease of long-standing (years!) chronic pains in lymph nodes
+ Notable but unstable, fluctuating improvements of swollen sinuses (chronic sinusitis)
+ Improvements of elevated resting heart rate and blood pressure readings.Notable improvement wrt fat maldigestion/malabsorption only set in three days after introducing the following:
Increasing Flu from 200mg to 300mg pd
Oregano essential oil, c. 4-5 drops in total pd (in food or oil)
Colloidal silica 2.8%, 15ml pd in a cup of water
Borax 0.5g/L in drinking waterThe propolis extract seemed of little systemic use and was removed from the regimen.
Nystatin has slowly been removed as well after c. 2.5 weeks because of the overlapping with oral AmB.Adverse effects of the Itr /Flu:
- Profound headaches (only in part relieved by psyllium with clinoptilolite)
- Enhanced depression, sadness, mental exhaustion. Especially initially, raising suspicions of cerebral fungal afflictions.
- Very dry skin and scalp. Very dry, dark-red, painful, peeling lips.
-> This is a known side effect of azoles. Especially fluconazole. MoA is unknown; something to do with renewal of skin cells. When this sides effect shows on the exterior skin I suspect GI cell renewal is affected, too.I'm no fan of the oregano essential oil. However, it appears to be one of the most powerful adjuvants. Obviously very bad for already damaged lips and the bottle always dispenses more drops per serving than I intend (should really use an eyedropper for it).
Intuitively I'd say the oregano EO and garlic are the two most powerful adjuvants.
I'm really underwhelmed by internal use of borax. If Travis was right and there's indeed substantial antifungal effect from it for an extensive part of the population I must suspect either a predominantly prophylactic effect (rather than therapeutic) and/or a highly varying susceptibility of fungal strains to boron.
I suspect the borax to dry out skin, too, and possibly making riboflavin profoundly unavailable (Boron forms very hydrophilic (easily washed out) complexes with B2).Currently:
Have stopped the 300mg Flu pd after 8 days and letting it fade out of the system over at least four days because it is said to negatively interact with the action of flucytosine.
Two days later: Strong joint pains, feeling very cold and insatiable which may all be immunological rebound effects by the Cyp27B1 inhibition (25-OH-D3 to 1,25-OH-D3) of Itr + Flu.
Three days later: Notable recession of the digestion improvements which had come with the 300mg pd. Return of chronic abdominal pains.Flucytosine is essentially 5-Fluorouracile, the bread-and-butter chemotherapy cytotoxin. It converts to 5-FU in susceptible yeast cells, yet to an unknown and varying degree also in the microbiome which is the mainly assumed cause of its adverse systemic effects.
-> As far as I could find out, neither Lactobacilli nor Bifidobacteria nor Clostridioides convert 5-FC to 5-FU but E. coli and Enterococci and Citrobacter do! Quite impossible therefore to avoid such intestinal conversion.
5-FC has a very short half-time and must be taken 4 times daily at regular intervals and peak serum concentrations ought to be measured three days into treatment. Empirically, the majority of treated patients exhibit peak and through serum concentrations out of range; either too high (toxicity!) or too low (treatment failure).Only today have I stumbled across differing treatment recommendations for oral AmB:
Some package slips say 100mg four times daily
yet in other countries the standard dosage is stated as 500mg four times daily. Both refer to exactly identical product compositions! What's up with this?
Maybe there's a profound lack of knowledge wrt dosage and 200-500mg AmB are more appropriate for (lower) GI effectivity in contrast to upper oropharyngeal treatment.
That could potentially render the coated 100mg AmB tablets escpecially daft and misleading because they are A. oropharyngally unavailable and B. the lowest bottom end and possibly insufficient dosage for targeting the lower GI system.
Given the lack of absorption and systemic side effects it'd therefore probably be wise to not slouch about with 100mg but to increase the oral AmB dosage to 200-500mg four times daily.@mauritio
Had read your old thread on the RPF again on riboflavin activity against Candida. Unfortunately, there are crucial caveats to it: That only applies to C. albicans.
C. glabrata, however, thrives on it. Throwing B2 or B1 or B3 at C. glabrata acts as a strong growth stimulant. C. glabrata (and Aspergillus spp.), in stark contrast to C. albicans, even feeds on bismuth subsalicylate (Pepto Bismol) / subcitrate to grow its biomass!
Unfortunately the C. glabrata is a definitely cultured part of my pathogenic mycobiome and I couldn't get an antimycogram on it.@Mauritio said:
My current working hypothesis is rotating and combining several anti fungals daily + keeping bile flowing.
If i don't rotate the antifungals they seem to loose effect surprisingly quickly.
But what is obvious from many studies, is that combining certain anti fungals can drastically increase their effectiveness. Nystatin is synergistic with thymoquinone and also thymol IIRC.I'd say to maintain a multi-pronged approach at all times. Afaik if resistancies develop they can rise within a couple of days. Don't know if any ineffective compound may prove to be effective again at a later time? Do strongly suggest to take biofilm breakers only in intermittent intervals as they can be way too harsh long-term.
@yerrag said:
But this should explain to me why it has become common practice for doctors to administer antifungal drugs after successfully treating a patient with antibiotics. But they cannot explain why
Thanks for sharing. What most wondrous and advanced country do you live in where doctors routinely prescribe antifungals with or following upon ABx treatments? Never happened to me. Never. And I have had incredibly absurd amounts and varieties of ABx. No medical practitioner ever mentioned fungi in over 20 years.
Hello! It looks like you're interested in this conversation, but you don't have an account yet.
Getting fed up of having to scroll through the same posts each visit? When you register for an account, you'll always come back to exactly where you were before, and choose to be notified of new replies (either via email, or push notification). You'll also be able to save bookmarks and upvote posts to show your appreciation to other community members.
With your input, this post could be even better 💗
Register Login