Random, interesting studies
-
It has been wondered how Helicobacter pylori actually spreads from human to human.
Beside the fecal-oral transmission in low hygienic standards, some few people have it in notable amounts even freely in their saliva, from where it can spread by aerosols, kissing or sharing drinks.Another transmission vector and reservoir, however, appears to be through oral, vaginal, food-borne and environmental spread of H.pylori-infected yeasts, which provide greatly enhanced protection to these bacteria, as shown by these Iranian researchers:
Vacuoles of Candida yeast as a specialized niche for Helicobacter pylori, 2014
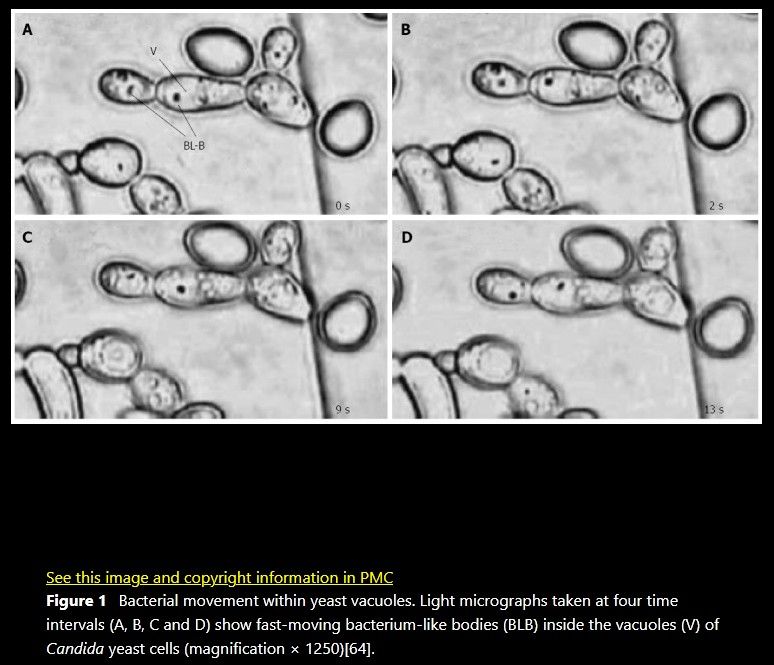
The internalized H.pylori also reproduces inside yeast vacuoles and when the yeast divide, H.pylori is imparted to the daughter generation.
Helicobacter pylori (H. pylori ) have been observed within yeast vacuoles by light and fluorescence microscopy, and their presence has been confirmed by the detection of H. pylori -specific genes and proteins in yeast extracts, such as VacA subunits, UreA, peroxiredoxin and thiol peroxidase.
Moreover, non-culturable H. pylori cells have been found in subsequent generations
of yeasts, indicating the generational transmission of the bacteria is part of the transfer of vacuolar content.
H. pylori are therefore well-equipped to establish in the vacuoles of yeast, which provide them with essential nutrients such as ergosterol for multiplication, as a pre-adaptation for invasion of human cells.Indeed, H. pylori-specific genes ureAB and babAB were detected in Candida yeasts from Iranian traditional breads (Sangak, Taftoon and Barbary), yogurt, banana skin, grape juice and quince jam, which carried vacuolar fast-moving and non-culturable BLBs (Figure 2)[87].
Thus, foodborne yeasts originating from the environment, which were once considered as harmless microorganisms when ingested through fermented foods such as dairy products[38,89], including kefir and kumis[94,95], could now be pinpointed as a public health problem source. In this regard, occurrence of yeast in food and environment can be considered as an important indicator of contamination with H. pylori and other pathogenic bacteria. Therefore, a key approach for the control of H. pylori infection may be to reduce the yeast content of foods through proper hygienic practice, especially by food handlers and during food processing[87]Would be interesting to know about the contamination in foods from "Western" sources and if H.pylori also infects saccharomyces boulardii/cerevisiae (baking yeast) and amoeba (water sources). And whether when we go buy goods which have not been baked like beer, (pasteurized) fermented foods or baking yeast (supplements?) they are free from intracellular bacteria?
There's a criticism of the study above which strongly questions the ability of bacteria to enter yeast cells. They do bring up amoeba and water supply, however:Interestingly, several articles in the literature have shown similarity in prevalence of Acanthamoeba in drinking water sampled from different geographical locations and the prevalence of H. pylori in patients[8-19]. While we cannot observe such overlap between yeast and H. pylori incidences, it is more logical to believe that yeast cannot be a reservoir of H. pylori but that Acanthamoeba can play such a role.
Indeed, in an earlier publication, the same Iranian researchers also showed commensalism in a co-culture of amoeba and H.pylori.
And they also found H.pylori in saccharomyces cerevisiae (baking + beer yeast) which was meant as a negative control - although in a less virulent, CagA-toxin free variation. Which could be coincidence or not. No testing for VacA-toxin was done in this context. -
-
SOD3 Overexpression completely reveres weight gain on a high fat diet.
It also improves insulin sensitivity, triglycerides, fatty liver and increases PGC1a and UCP2.Interesting that a simple enzyme that reduces oxidative stress is so impactful.
Even though antioxidants don't get the best rap in the peat world. This study is similar to the ones using selegiline, ergothioneine or catalase overexpession, in the sense that their main mechanism of action is protection from oxidative stress. -
"Platelet COX inhibition was nearly complete already at 37.5 mg aspirin daily, as evidenced by >98% suppression of serum thromboxane B2 ..."
-
@Mauritio Bro this is insane.
https://pubmed.ncbi.nlm.nih.gov/18505478/
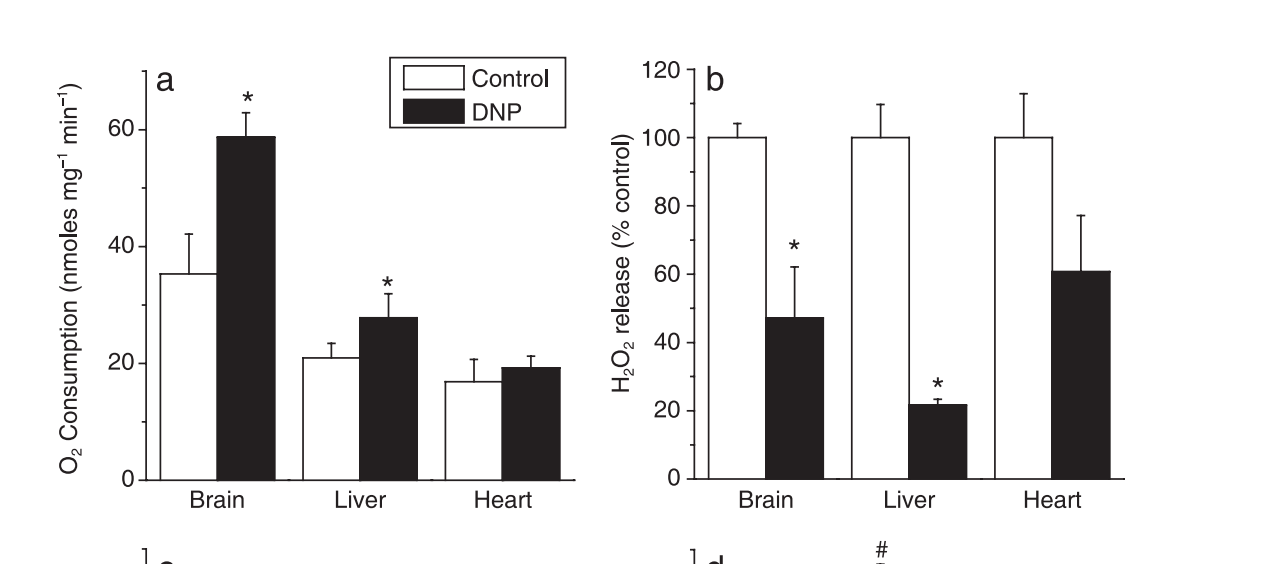
If the mice were drinking 3.2ml of water a day, that is 0.032mg of DNP.
They weighed around 0.0475kg
So 0.67mg / kgHED is 0.0536mg per kg
80kg man: 4mg
-
@alfredoolivas yes lve posted this and similar studies on X and maybe also on here.
Microdose DNP is very beneficial. Its also being researched to treat Ms. -
@Mauritio Yeah I was thinking of your post and looked into it a but
-
Apple polyphenols protect from aspirin induced stomach damage.
https://pubmed.ncbi.nlm.nih.gov/25069887/
https://pubmed.ncbi.nlm.nih.gov/18482463/Honey and propolis help as well.
https://www.mdpi.com/2072-6643/13/9/3169
https://www.sciencedirect.com/science/article/abs/pii/S2214785321029254The protection always seems to stem from the polyphenol content of those foods. So I suspect that eating anything that has alot of polyphenols with the aspirin should work. Berries, fruits, or a glass of Orange juice.
-
@Mauritio said in Random, interesting studies:
anything that has alot of polyphenols with the aspirin should work.
Yes, to counteract excess oxidation and then inflammation. But we need to optimize mucin thickness with glutamine (and taurine to counteract the excitotoxcity in the brain).
I take half a teaspoon of taurine and the same with glutamine powder, one hour before bedtime, when I feel a stomach acidity. No glutamine if you suffer from dysbiosis (suspicion of candidiasis: it feeds the bacteria).
When it's nervous, L-theanine 225 mg and 1 tsp collagen do the job (cramp). Never take SSRS as a usual med... -
"The effect of vitamin A supplementation on plasma estrogen and progesterone were studied in pregnant women. While there was no change in the estrogen concentration, the mean increment in plasma progesterone in the supplemented group was significant when compared to the unsupplemented group. It is suggested that vitamin A supplementation to undernourished pregnant women may have beneficial effect on feto-placental function."
https://pubmed.ncbi.nlm.nih.gov/1856040/ -
Now here's something controversial and interesting from Cell:
To take probiotics post-antibiotic treatmentcanwill inhibit restoration of one's microbiome in contrast to simply letting things run its course without any post-antibiotic intervention (if one's lucky enough to not get a CDI, of course. Yet the course for that may have been set already during Abx treatment, we don't really know if probiotics after Abx can rescue that).
A much more effective could be "autologous fecal matter transplant". No foreign donor required.
Collecting, filtering, liquefying and freezing one's pre-antibiotic healthy microbiome and using this once on day 0 after antibiotic treatment.
Like in hamsters: Eating your own shit. This enriches the (mostly preserved) endogenous microbiome reserves and puts them back from the end to the more proximal parts of the digestive system.Compared to spontaneous post-antibiotic recovery, probiotics induced a markedly delayed and persistently incomplete indigenous stool/mucosal microbiome reconstitution and host transcriptome recovery toward homeostatic configuration, while aFMT induced a rapid and near-complete recovery within days of administration.
In rodent experiments, the degree of mucosal colonization with human-specific probiotics even after antibiotic pretreatment was los. Pointing yet again to a huge importance of specifity between host species and strain.
I.e. rodent studies for testing probiotic benefits in humans are quite garbage?
The study went on to human volunteers with the same and apparently very reasonable 11-strain Lactobacillus + Bifidobacterium probiotic blend ("Supherb Bio-25", 25 billion CFU twice daily):Following antibiotic treatment, seven participants were followed by watchful waiting for spontaneous microbiome reconstitution, six participants received aFMT (STAR Methods), and eight participants received the aforementioned 11-strain probiotics preparation administered bi-daily for a period of 4 weeks (Figure 3A).
participants from the aFMT arm received an intrajejunal infusion of 150 ml of processed and liquefied stool (on day 0), which had been obtained from the participant prior to the antibiotics therapy
In the spontaneous recovery group, significant differences in stool composition compared to baseline abated within 21 days of antibiotics cessation (Figure 4B). In contrast, probiotics-consuming individuals did not return to their baseline stool microbiome configuration by the end of the intervention period (day 28), and dysbiosis was maintained even 5 months after probiotics cessation, with all stool samples collected through day 180 remaining significantly different from baseline
dun- dun dun dun.
And here's another interesting find from nature microbiology, where they blasted volunteers with the three "last-resort" antibiotics meropenem, gentamicin and vancomycin:
Recovery of gut microbiota of healthy adults following antibiotic exposure, 2018
The gut microbiota of the subjects recovered to near-baseline composition within 1.5 months, although 9 common species, which were present in all subjects before the treatment, remained undetectable in most of the subjects after 180 days.
That latter part sort of negates the first statement, doesn't it?
Finally, some species detected at D0 were not detected again within the study time frame.
These included: (1) members of genus Bifidobacterium that are considered pathogen-protective and immunostimulatory;
2) butyrate producers such as Coprococcus eutactus and Eubacterium ventriosum and
(3) methane-producing Methanobrevibacter smithii associated with the efficient digestion of polysaccharides.Remarkably, only two F. prausnitzii strains were able to recover by D180, another six could not recover through the study period (Supplementary Fig. 3), reflecting the different recovery capacities between conspecific strains.